Blood – Definition, Composition, functions, Formation, Types & More
Blood, the life-sustaining fluid coursing through our veins, serves as the body’s primary transport system. It delivers essential nutrients and oxygen to cells, while removing waste products and carbon dioxide. This vital fluid also plays a crucial role in immune defense, clotting, and maintaining homeostasis. In this article, we will explore the composition, functions, and importance of blood, shedding light on its integral role in maintaining human health and vitality.
Definition of Blood
Blood is a specialized bodily fluid that performs essential functions to sustain life. It circulates through the body’s cardiovascular system, delivering vital substances and removing waste products. Here are the primary components and functions of blood
Composition of Blood
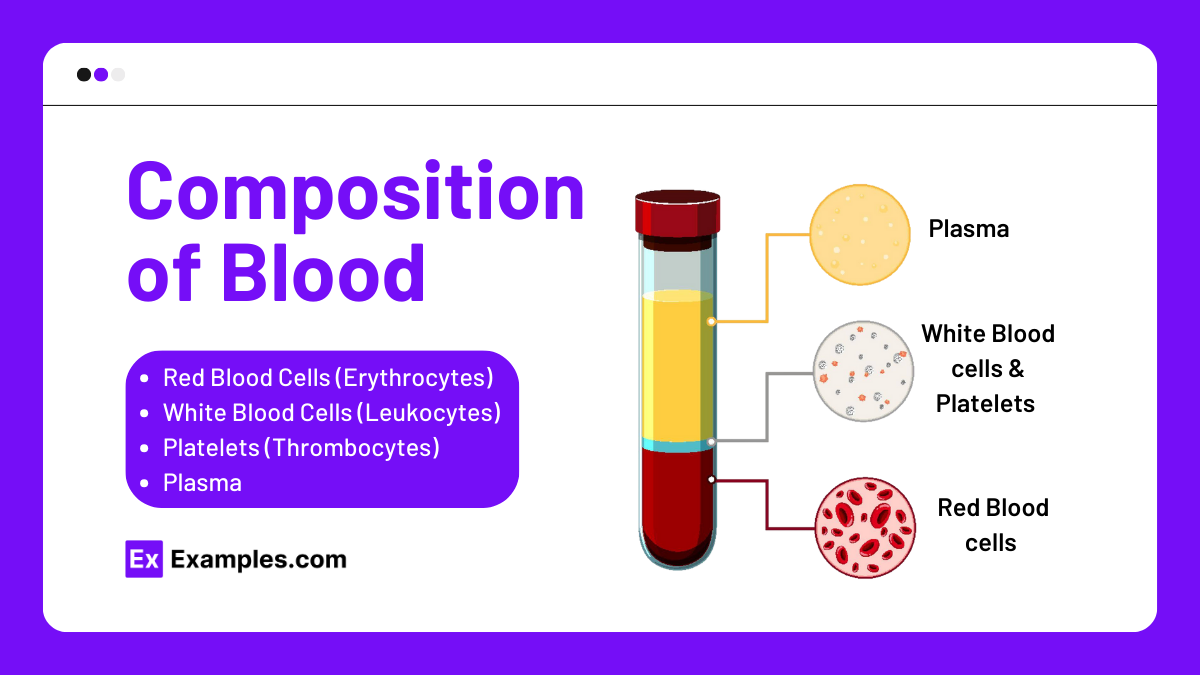
Blood is composed of four main components: red blood cells, white blood cells, platelets, and plasma. Each component plays a unique and essential role in maintaining the body’s health and functionality.
Red Blood Cells (Erythrocytes)
Structure and Function: Red blood cells are biconcave, disc-shaped cells that lack a nucleus. Their primary function is to transport oxygen from the lungs to the body’s tissues and return carbon dioxide from the tissues to the lungs. Hemoglobin, a protein within red blood cells, binds to oxygen and facilitates this transportation.
Production: Red blood cells are produced in the bone marrow through a process called erythropoiesis. This process is regulated by erythropoietin, a hormone produced by the kidneys in response to low oxygen levels.
Lifespan: The average lifespan of a red blood cell is about 120 days. Old or damaged red blood cells are removed from circulation by the spleen and liver.
White Blood Cells (Leukocytes)
Types and Functions: White blood cells are crucial for the immune system. They protect the body against infections and foreign invaders. There are several types of white blood cells, each with specific functions:
- Neutrophils: These are the most abundant type of white blood cells. They are the first responders to infection and are particularly effective against bacteria and fungi.
- Lymphocytes: There are two main types: B cells and T cells. B cells produce antibodies that target pathogens, while T cells destroy infected or cancerous cells.
- Monocytes: These cells differentiate into macrophages and dendritic cells in tissues, where they engulf and digest pathogens and dead cells.
- Eosinophils: These cells combat multicellular parasites and participate in allergic reactions.
- Basophils: These are involved in inflammatory responses and release histamine during allergic reactions.
Lifespan: The lifespan of white blood cells varies greatly depending on the type. Some may live for a few hours to a few days, while others, like memory T cells, can live for years.
Platelets (Thrombocytes)
Structure and Function: Platelets are small, disc-shaped cell fragments without a nucleus. Their primary function is to prevent bleeding by forming blood clots. When a blood vessel is injured, platelets adhere to the site, aggregate, and work with clotting factors to form a stable clot that seals the wound.
Production: Platelets are produced in the bone marrow from large cells called megakaryocytes. Each megakaryocyte can release thousands of platelets into the bloodstream.
Lifespan: Platelets have a relatively short lifespan of about 7-10 days. They are continuously replenished by the bone marrow.
Plasma
Composition and Function: Plasma is the liquid component of blood, making up about 55% of its total volume. It is primarily composed of water (about 90%) but also contains proteins, electrolytes, hormones, nutrients, and waste products.
- Proteins: The main proteins in plasma include albumin, which maintains osmotic pressure and transports substances; globulins, which include antibodies and transport proteins; and fibrinogen, which is essential for blood clotting.
- Electrolytes: These include sodium, potassium, calcium, and chloride, which help regulate nerve and muscle function, hydration, blood pH, and blood pressure.
- Hormones and Nutrients: Plasma transports hormones, glucose, amino acids, and lipids to various parts of the body.
- Waste Products: Plasma carries metabolic waste products like urea and carbon dioxide to the kidneys and lungs for excretion.
Functions of Blood
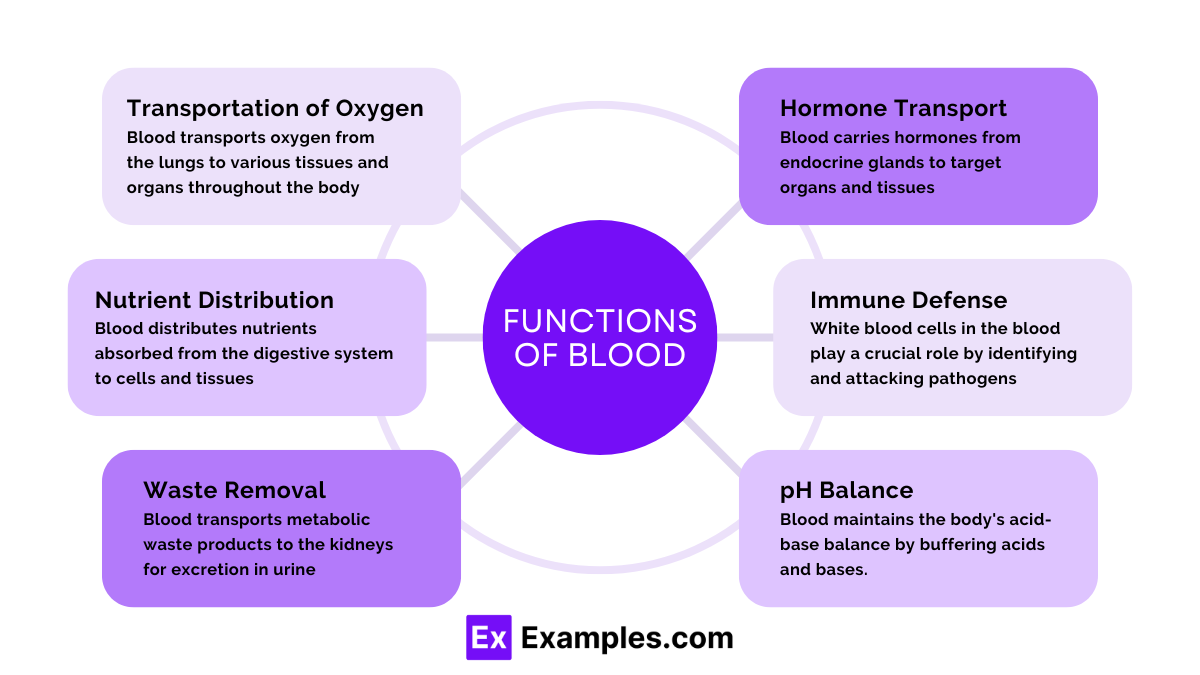
Transportation of Oxygen
Blood transports oxygen from the lungs to various tissues and organs throughout the body. Hemoglobin in red blood cells binds to oxygen molecules and releases them where needed.
Removal of Carbon Dioxide
Blood carries carbon dioxide, a waste product of metabolism, from the tissues to the lungs for exhalation. This helps maintain the body’s pH balance.
Nutrient Distribution
Blood distributes nutrients absorbed from the digestive system to cells and tissues. These nutrients include glucose, amino acids, fatty acids, and vitamins.
Waste Removal
Blood transports metabolic waste products, such as urea and creatinine, to the kidneys for excretion in urine, thus preventing toxic accumulation.
Regulation of Body Temperature
Blood helps regulate body temperature by distributing heat generated by metabolic processes throughout the body and to the skin for dissipation.
Hormone Transport
Blood carries hormones from endocrine glands to target organs and tissues, facilitating communication and regulation of various bodily functions.
Immune Defense
White blood cells in the blood play a crucial role in the immune response by identifying and attacking pathogens, such as bacteria and viruses, and producing antibodies.
Clotting Mechanism
Blood contains platelets and clotting factors that initiate the clotting process, preventing excessive blood loss from injuries and promoting wound healing.
pH Balance
Blood maintains the body’s acid-base balance by buffering acids and bases. This is crucial for normal cellular function and enzyme activity.
Water Balance
Blood helps regulate the body’s fluid balance by absorbing and distributing water, ensuring that cells and tissues remain hydrated.
Transport of Gases
In addition to oxygen and carbon dioxide, blood transports other gases like nitric oxide, which plays a role in vascular dilation and blood pressure regulation.
Nutrient Reserve
Blood serves as a reservoir for nutrients such as glucose and lipids, which can be mobilized during periods of fasting or increased demand.
Regulation of Electrolytes
Blood maintains the balance of electrolytes such as sodium, potassium, and calcium, which are essential for nerve function, muscle contraction, and cellular activities.
Protection Against Toxins
Blood detoxifies harmful substances by transporting them to the liver for detoxification and subsequent excretion.
Support for Metabolism
Blood provides the necessary substrates for cellular metabolism and removes the byproducts of metabolic processes, ensuring efficient energy production and use.
Formation of Blood
Blood formation, or hematopoiesis, is a complex process by which blood cells are produced in the body. This essential biological process occurs primarily in the bone marrow, but it also involves the liver and spleen, particularly during fetal development. The following sections explain the stages and mechanisms involved in the formation of blood.
Hematopoiesis Process
- Stem Cells:
- Hematopoiesis begins with hematopoietic stem cells (HSCs), which are multipotent cells found in the bone marrow.
- These stem cells have the ability to differentiate into various types of blood cells.
- Differentiation:
- HSCs undergo a process of differentiation where they become either myeloid progenitor cells or lymphoid progenitor cells.
- Myeloid progenitor cells give rise to red blood cells (erythrocytes), platelets (thrombocytes), and various white blood cells (granulocytes and monocytes).
- Lymphoid progenitor cells differentiate into lymphocytes, which are crucial for the immune response.
- Erythropoiesis:
- The formation of red blood cells is called erythropoiesis.
- This process is stimulated by the hormone erythropoietin, primarily produced by the kidneys in response to low oxygen levels.
- The precursor cell for red blood cells, the proerythroblast, undergoes several stages before becoming a mature erythrocyte.
- Leukopoiesis:
- The formation of white blood cells is known as leukopoiesis.
- This includes the development of granulocytes (neutrophils, eosinophils, basophils), monocytes, and lymphocytes.
- Each type of white blood cell has a specific precursor and maturation pathway.
- Thrombopoiesis:
- The production of platelets, or thrombopoiesis, involves the differentiation of megakaryocytes from myeloid progenitor cells.
- Platelets are essential for blood clotting and wound healing.
Factors Influencing Hematopoiesis
- Growth Factors and Cytokines:
- Various growth factors, such as granulocyte colony-stimulating factor (G-CSF), granulocyte-macrophage colony-stimulating factor (GM-CSF), and interleukins, play critical roles in the proliferation and differentiation of blood cells.
- Bone Marrow Microenvironment:
- The bone marrow provides a supportive environment for hematopoiesis through stromal cells, extracellular matrix, and a network of blood vessels.
Stages of Blood Cell Development
| Blood Cell Type | Progenitor Cells | Mature Cells |
|---|---|---|
| Erythrocytes | Proerythroblast | Erythrocyte (Red Blood Cell) |
| Platelets | Megakaryoblast | Thrombocyte (Platelet) |
| Neutrophils | Myeloblast | Neutrophil |
| Eosinophils | Myeloblast | Eosinophil |
| Basophils | Myeloblast | Basophil |
| Monocytes | Monoblast | Monocyte |
| Lymphocytes | Lymphoblast | B-Cell, T-Cell, NK Cell |
Blood Types
Blood types are classifications of blood based on the presence or absence of specific antigens on the surface of red blood cells. These antigens can trigger an immune response if they are foreign to the body. Understanding blood types is crucial for safe blood transfusions, organ transplants, and understanding certain medical conditions.
The ABO Blood Group System
The ABO blood group system is the most important blood type system in human blood transfusion. It is determined by the presence or absence of two antigens, A and B, on the surface of red blood cells.
- Type A: Has A antigens on the surface of the red blood cells and anti-B antibodies in the plasma.
- Type B: Has B antigens on the surface of the red blood cells and anti-A antibodies in the plasma.
- Type AB: Has both A and B antigens on the surface of the red blood cells and no anti-A or anti-B antibodies in the plasma. Type AB is known as the universal recipient.
- Type O: Has no A or B antigens on the surface of the red blood cells but has both anti-A and anti-B antibodies in the plasma. Type O is known as the universal donor.
The Rh Blood Group System
The Rh blood group system is the second most significant blood type classification. It is based on the presence or absence of the Rh antigen (also known as the D antigen).
- Rh-positive (Rh+): Has the Rh antigen on the surface of the red blood cells.
- Rh-negative (Rh-): Does not have the Rh antigen on the surface of the red blood cells.
Combining the ABO and Rh systems, we get the following blood types: A+, A-, B+, B-, AB+, AB-, O+, and O-.
Blood Type Compatibility
Blood Transfusions
- Type O-: Universal donor for red blood cells.
- Type AB+: Universal recipient for red blood cells.
- Plasma Compatibility:
- AB: Universal donor for plasma.
- O: Universal recipient for plasma.
Organ Transplants
Blood type compatibility is also crucial in organ transplants. An incompatible blood type can lead to organ rejection.
Blood Type Distribution
Blood type distribution varies among different populations and ethnic groups. Here is a general distribution of blood types in the United States:
| Blood Type | Percentage (%) |
|---|---|
| O+ | 37.4 |
| O- | 6.6 |
| A+ | 26.3 |
| A- | 5.7 |
| B+ | 8.5 |
| B- | 1.5 |
| AB+ | 3.4 |
| AB- | 0.6 |
Importance of Blood Types
- Blood Transfusions: Matching the donor’s and recipient’s blood types prevents adverse reactions.
- Pregnancy: Rh compatibility between mother and fetus is crucial to prevent hemolytic disease of the newborn.
- Forensic Science: Blood types can help in identifying individuals in forensic investigations.
- Disease Susceptibility: Certain blood types are linked to a higher or lower risk of specific diseases.
Color of Blood
Human Blood Color
Red Coloration
Human blood is red, but the shade can vary:
- Oxygenated Blood: Bright red. This is the color of arterial blood, which is rich in oxygen after being pumped from the lungs.
- Deoxygenated Blood: Darker red. This is the color of venous blood, which has released its oxygen to the tissues and is returning to the lungs for reoxygenation.
The red color of blood is due to the presence of hemoglobin, a protein in red blood cells. Hemoglobin contains iron, which binds to oxygen. The iron-oxygen complex absorbs and reflects light in a way that gives blood its red color.
Why Hemoglobin Makes Blood Red
Hemoglobin is composed of four subunits, each containing an iron atom embedded in a heme group. When oxygen binds to the iron in hemoglobin, it causes a change in the shape of the hemoglobin molecule, which alters its light absorption properties. This change in light absorption is what causes oxygenated hemoglobin to appear bright red.
Blood Colors in Other Animals
The color of blood varies across the animal kingdom due to differences in the respiratory pigments used to transport oxygen.
- Red Blood (Hemoglobin-based):
- Humans and Most Vertebrates: Use hemoglobin, resulting in red blood.
- Blue Blood (Hemocyanin-based):
- Arthropods and Mollusks: Use hemocyanin, which contains copper instead of iron. Hemocyanin is blue when oxygenated.
- Green Blood (Chlorocruorin-based):
- Some Annelids: Use chlorocruorin, which is green when dissolved in plasma.
- Violet Blood (Hemerythrin-based):
- Some Marine Invertebrates: Use hemerythrin, which is violet-pink when oxygenated.
Misconceptions About Blood Color
- Venous Blood Appearing Blue: Veins appear blue through the skin due to the way light penetrates and scatters through the skin, not because the blood itself is blue. Veins are closer to the surface and the skin and subcutaneous fat layers absorb more red light and reflect blue light, making veins appear blue.
- Blood Outside the Body: Blood that is exposed to air rapidly becomes oxygenated, turning bright red. Even deoxygenated blood from a vein will appear red when it is outside the body.
Color Changes in Pathological Conditions
Certain medical conditions can cause changes in blood color:
- Methemoglobinemia: Blood turns a brownish color due to the presence of methemoglobin, an oxidized form of hemoglobin that cannot bind oxygen.
- Cyanosis: A bluish color of the skin and mucous membranes due to low oxygen levels in the blood, although the blood itself remains dark red.
Temperature Regulation in Blood
Temperature regulation is a crucial physiological process that helps maintain the body’s core temperature within a narrow, optimal range, typically around 37°C (98.6°F). Blood plays a vital role in this thermoregulation through several mechanisms.
Mechanisms of Temperature Regulation
- Heat Distribution:
- Blood as a Heat Conductor: Blood absorbs heat generated by metabolic processes in muscles and organs and distributes it throughout the body.
- Equalizing Temperature: This helps in equalizing temperature differences between different body parts, maintaining a stable internal environment.
- Vasodilation and Vasoconstriction:
- Vasodilation: When the body needs to dissipate heat, blood vessels, particularly near the skin surface, dilate (widen). This increases blood flow to the skin, allowing more heat to be released into the surrounding environment.
- Vasoconstriction: Conversely, when the body needs to conserve heat, blood vessels constrict (narrow), reducing blood flow to the skin and extremities, thereby minimizing heat loss.
- Sweating:
- Heat Loss Through Evaporation: Blood flow to sweat glands increases during high temperatures. The sweat produced evaporates from the skin surface, carrying away heat and cooling the body.
- Shivering:
- Heat Generation: When the body is cold, muscles contract involuntarily (shivering), producing heat through increased metabolic activity. Blood helps distribute this generated heat throughout the body.
Blood Flow and Thermoregulation
- Skin Blood Flow:
- Thermoregulatory Organ: The skin acts as a major thermoregulatory organ. Blood flow to the skin increases or decreases depending on the body’s need to lose or retain heat.
- Arteriovenous Anastomoses: These specialized blood vessels bypass capillaries to regulate blood flow to the skin, playing a critical role in temperature control.
- Core and Peripheral Temperature:
- Core Temperature Maintenance: Blood helps maintain a stable core temperature by redistributing heat from the body’s core to the periphery and vice versa.
- Peripheral Temperature: The temperature of the extremities can vary significantly, allowing the body to adapt to different environmental conditions.
Physiological Responses to Temperature Changes
- Heat Stress:
- Increased Heart Rate: To facilitate heat dissipation, the heart rate increases, pumping more blood to the skin and extremities.
- Sweating and Vasodilation: Enhanced sweating and vasodilation promote heat loss through evaporation and radiation.
- Cold Stress:
- Decreased Blood Flow to Extremities: Vasoconstriction reduces blood flow to the skin and extremities, conserving core body heat.
- Increased Metabolic Rate: The body increases metabolic activity to generate more heat.
Impact of Blood Volume and Composition
- Blood Volume:
- Maintaining Adequate Circulation: Adequate blood volume is essential for effective temperature regulation. Dehydration can impair the body’s ability to regulate temperature, leading to conditions such as heat stroke.
- Blood Composition:
- Plasma and Electrolytes: The plasma and electrolyte balance in the blood play a crucial role in thermoregulation, affecting sweat production and overall fluid balance.
Blood Disorders
| Disorder | Affected Blood Component | Symptoms | Causes |
|---|---|---|---|
| Iron-Deficiency Anemia | Red Blood Cells | Fatigue, weakness, pale skin | Lack of iron |
| Sickle Cell Disease | Red Blood Cells | Pain, potential organ damage | Genetic mutation |
| Acute Lymphocytic Leukemia | White Blood Cells | Fever, fatigue, frequent infections | Unknown, genetic factors |
| Hodgkin Lymphoma | White Blood Cells | Swollen lymph nodes, night sweats | Genetic mutations, Epstein-Barr virus |
| Immune Thrombocytopenia | Platelets | Easy bruising, excessive bleeding | Autoimmune response |
| Hemophilia A | Platelets (clotting factor) | Excessive bleeding, joint pain | Genetic mutation (factor VIII deficiency) |
| Von Willebrand Disease | Platelets (clotting factor) | Prolonged bleeding, nosebleeds | Genetic mutation |
Facts About Blood
- Blood Composition: Blood is composed of red blood cells, white blood cells, platelets, and plasma. Plasma, which makes up about 55% of blood, is mostly water but also contains proteins, glucose, hormones, and waste products.
- Red Blood Cells: Red blood cells (RBCs) are responsible for carrying oxygen from the lungs to the rest of the body and returning carbon dioxide to the lungs for exhalation. RBCs contain hemoglobin, a protein that binds to oxygen.
- White Blood Cells: White blood cells (WBCs) are crucial for the immune system. They help fight infections by attacking bacteria, viruses, and other foreign invaders. There are several types of WBCs, including neutrophils, lymphocytes, and monocytes.
- Platelets: Platelets are small cell fragments that play a key role in blood clotting. When you get a cut, platelets gather at the site and form a clot to stop the bleeding.
- Blood Types: There are four main blood types: A, B, AB, and O. Each type can be positive or negative, depending on the presence of the Rh factor. The most common blood type is O positive, while the rarest is AB negative.
- Universal Donor and Recipient: People with O negative blood are considered universal donors because their blood can be given to anyone. AB positive individuals are universal recipients because they can receive blood from any type.
- Blood Volume: An average adult has about 5 liters (1.3 gallons) of blood, which makes up about 7-8% of their body weight.
- Blood Transfusion: Blood transfusions can save lives by replacing lost blood. Donated blood is carefully screened and matched to the recipient’s blood type to prevent adverse reactions.
- Lifespan of Blood Cells: Red blood cells have a lifespan of about 120 days, after which they are broken down and recycled by the spleen and liver. White blood cells can live from a few days to several years, depending on the type.
- Blood Regeneration: The body is capable of regenerating lost blood. After donating blood, it takes about 4-6 weeks for the body to replace the plasma and about 8 weeks to replace the red blood cells.
- Oxygen Transport: Hemoglobin in red blood cells can carry four molecules of oxygen. When hemoglobin binds to oxygen, it forms a bright red compound called oxyhemoglobin.
- Blood Vessels: The circulatory system includes a vast network of blood vessels, which, if laid end-to-end, would stretch about 60,000 miles. This network includes arteries, veins, and capillaries.
- Antibodies in Blood: The plasma in blood contains antibodies that help fight infections. These antibodies are part of the body’s immune response and are crucial for identifying and neutralizing pathogens.
- Blood Donation: Donating blood is a simple and safe process that can save up to three lives with each donation. Blood banks and hospitals constantly need donations to maintain an adequate supply.
- Blood and Evolution: The ability to transport oxygen efficiently through blood has been a key factor in the evolution of complex organisms, enabling higher metabolic rates and the development of larger, more complex bodies.
What is blood?
Blood is a vital fluid that circulates through the body, delivering oxygen and nutrients to cells and removing waste products.
What are the main components of blood?
Blood consists of red blood cells, white blood cells, platelets, and plasma.
What is the function of red blood cells?
Red blood cells transport oxygen from the lungs to the rest of the body and carry carbon dioxide back to the lungs for exhalation.
What do white blood cells do?
White blood cells are crucial for the immune system, protecting the body against infections and foreign invaders.
What role do platelets play?
Platelets help with blood clotting, preventing excessive bleeding when injuries occur.
What is plasma?
Plasma is the liquid component of blood, containing water, salts, enzymes, antibodies, and other proteins.
How is blood produced?
Blood cells are produced in the bone marrow, a spongy tissue inside bones.
What is anemia?
Anemia is a condition where there is a deficiency of red blood cells or hemoglobin, leading to fatigue and weakness.
What causes high blood pressure?
High blood pressure can be caused by genetics, poor diet, lack of exercise, and stress.
How can you maintain healthy blood?
Maintain healthy blood by eating a balanced diet, staying hydrated, exercising regularly, and avoiding smoking.



