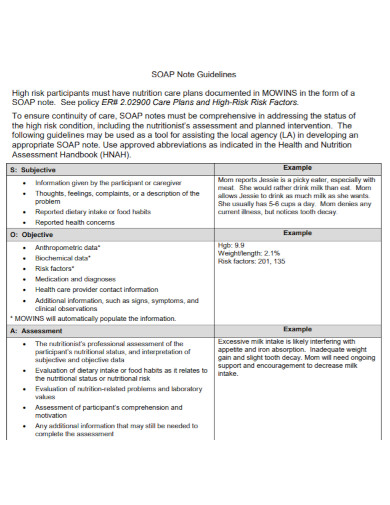
Comprehensive Soap Note Examples to Download
Men and women working as nurses or any position in the medical field or health care would know that assessment notes are important. Having to write everything down without missing a single information is necessary as well. As notes and reports are very important in this type of field, one must be able to know how to juggle with writing, assessing and giving out a plan to help their patients. This is where a SOAP note comes to play. To know more about what this is, how helpful it is as well as how to write one, check out the article.
3+ Comprehensive Soap Note Examples
1. Comprehensive Soap Note Template
2. General Comprehensive Soap Note
3. Student Comprehensive Soap Note
4. Comprehensive Soap Note in PDF
What Is a Comprehensive Soap Note?
A comprehensive SOAP note is a type of assessment tool used by nurses or anyone in health care. This assessment note gives out the specific information that would be necessary to assess and plan out the medical journey of a patient. A comprehensive SOAP note is more specific than a normal SOAP note as this type gives out a longer narrative of the assessment. In addition to that, it also takes in to all accounts of subjective, objective information needed to make the assessment. Lastly, a comprehensive SOAP note is a helpful tool when it comes to knowing the medical history of a patient. As this gives out the necessary information in the order of how it should be done. Starting with the subjective information and moving to the objective information.
A SOAP note is also a method used to help nurses, physicians and anyone working in the field as a way to save up time in understanding the patient’s medical history. It is also a simpler way to do notes while doing rounds. It is also a helpful way for students or medical practitioners to be able to observe, assess and make note on the medical issues without having to stop and write. The reason why a soap note can also be helpful is because it keeps practitioners time to give out an assessment without having to stop and ask the patient of their problems. It is also a good way to be able to find a solution without having to waste precious time. However, there are also things to reconsider when doing this type of method. Lastly, a comprehensive note is a specific and straight to the point type of assessment that speaks out the information given by patients as a way of understanding their medical history.
How to Write a Comprehensive Soap Note
Check these out. How to write a comprehensive soap note. These tips would surely be of help especially for those who may still be planning on writing one. This could also be additional information for those who have already written one.
1. Be Specific with Your Notes
When you write your soap note, always remember that the more specific you are, the better information can be gathered from it. The reason this is better is because not all general information can give out the true outcome of the medical history of a patient. As well as getting more specific details helps with knowing what can be done to help. Basically, the more specific you are, the better chances of understanding and assessing the situation.
2. Separate Your Keywords from Your Main Topic
This often gets confusing. And since it is necessary to always be on the go when you are writing your SOAP notes. The best way for you to be able to get everything in order is by making keywords. However, you must separate your keywords from your main topic. The reason for having to write your keywords is to help you get started on your main topic. Keywords are simply the stepping stone as to what you may be planning on expounding.
3. Use Examples to Back Up Your Notes
To make your notes even more realistic or understandable, add some examples to it. Your examples must also be based on the observations you made.
4. Use Jargon That Fit Your Field
Avoid having to use jargon that may be too difficult to understand. As well as jargon that may be too general or obvious. Your choice of words should be made possible to be understood by people in your field. They should also be made to avoid misunderstandings between patients and yourself.
5. Keep It Professional
Something to remember at all times. When you do your soap notes, always keep a professional tone and practice. Even when you are interacting with your patients, always remember to keep it professional. Avoid having to show your notes to them as this is between you and your superiors.
FAQs
What does SOAP mean in comprehensive SOAP notes?
SOAP is an acronym for Subjective, Objective, Assessment, Plan. This comprehensive soap note is mainly used by anyone working in the medical or health care field. It is used as a simple guided note for them to report to their superiors of the observations they have done. As well as to have a plan on what can be done to solve potential problems their patients may suffer.
How useful can this type of notes be for nurses?
This type of note helps you observe and at the same time take down notes. It is a method used to keep healthcare workers write and observe without having to stop what they are doing to write down what they have noticed. As this often takes a lot of time if they had to stop and write. This method of notes can also be used as a way of reporting what you have done to your superiors.
Are my notes okay to be seen by my patients or are they reserved for my supervisors?
Your notes are only to be given to your head or your supervisors. Your notes are not supposed to be read by your patients as this is your observation of how they feel and act.
What other way could I take down notes without any problem?
Use keywords. Using your own keywords as long as you understood the topic or the information can also help.
Is it necessary to use jargon that fits my field?
Using jargon that may be too difficult for others to understand is a huge problem. Rather, find words that are suitable in your field, as well as it is understandable to all.
Observing, taking down notes and reporting can be a tough thing to juggle. Especially if you are working as a healthcare worker or a nurse at a hospital. You must always be on your toes and alert for anything possible to happen. With this issue, it is difficult enough to have to take down more notes while observing your patients for any possible change in them. This is where the soap note comes in. It helps you list down the desired keywords for you, and you are able to write your own full sentence from the keywords. Not only that, this type of method is very helpful to those working as it gives them an overview of the assessment being done to help solve their problems.