10+ Clinical Quality Management Plan Examples to Download
Clinical management is a type of health care service that is used as a powerful tool in offering the best health assistance. Today, what we consider as the basic theory of clinical management is the heath manpower formation. Thus, it is also considered as an important aspect to correct health system. This has been proven necessary in collecting indicators and in clinical departments also. As of the moment, the development of clinical management is not the same to any regions and in any clinical departments. To use this tool means enhancing our daily clinical practice to improve the quality of health assistance.
10+ Clinical Quality Management Plan Examples
1. Clinical Quality Management Plan Fact Sheet
2. Clinical Quality Management Plan Template
3. Basic Clinical Quality Management Plan
4. Standard Clinical Quality Management Plan
5. Clinical Quality Management Committee Plan
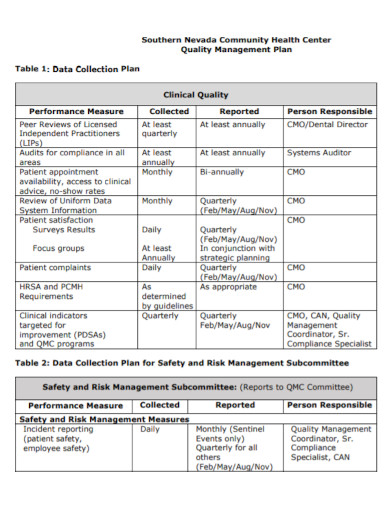
6. Clinical Quality Management Data Collection Plan
7. Printable Clinical Quality Management Plan
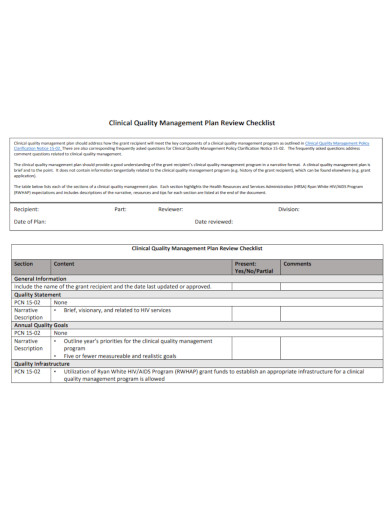
8. Clinical Quality Management Plan Checklist
9. Clinical Quality Management Work Plan
10. Professional Clinical Quality Management Plan
11. Clinical Quality Management Statement Plan
Clinical Management Plan Definition
A clinical quality management plan is a plan of treatment for a specific patient that does a legal boundary of his or her medication and the parameters of prescribed responsibility. It serves as a cornerstone between the physician and the supplementary prescriber. It can be drafted by either the supplementary prescriber or an independent prescriber. However, they should be able to agree to it before they are going to prescribe it to the patient.
This type of plan forms a foundation between a patient’s treatment after the initial admission. This must be based on the medical condition of a patient or in his or her treatment preferences as well as the recommendations given by the attending physician, nurse and other health care providers. Writing a clinical management plan would require to give full attention to the details and full understanding over the condition and treatment of the patient. The plan must contain the date as to when the treatment began and the classification of the medications that has being administered.
Steps in Writing a Clinical Management Plan
1. Obtain a clinical management plan template – you should get a copy of the template from your health care institution. This is a type of form that allows recording and presenting various information.
2. Collect all the patient’s information – the patient’s information includes name, age, patient ID, and the information about her medical condition and treatment.
3. Make sure that the patient’s information is placed in the upper left corner of the form.
4. Include the name and title of independent prescriber as well as the supplementary prescriber – this could mean another physician, hospice, nurse or health care provider.
5. Describe the condition and the objective of the treatment.
6. Write down the medications being prescribed – make sure that you put all the details about the patient’s medication by simply describing about what type of preparation to use, dosage, and indications that the medication will treat.
7. Record the protocols that support your clinical management plan – this refers to the allergy warnings, physiotherapy, instructions such as psychotherapy instructions and dietary instructions that is incorporated with the situation of the patient.
8. Add instructions about how the independent and supplementary prescribers can access the records of the patient.
9. Add instructions about how would the clinical management plan will be reviewed and monitored from time to time.
10. Do not forget to include the date as to when does the plan was agreed by both the prescribers and the patient.
11. Affix signatures of both the supplementary and independent prescribers.
FAQs
Is a clinical management plan a legal document?
There are no legal restrictions when it comes to the clinical condition being dealt with the supplementary prescriber.
What does it mean by supplementary prescribing?
Supplementary prescribing means having a partnership with an independent prescriber and a supplementary prescriber for the implementation of a CMP under a patient’s agreement.
What do clinical managers do?
Clinical managers do manage the daily activities inside the health care facility. They are handling both the medical and administrative aspects.
The concept of having a plan is essential especially if you are handling health care services for patient with big needs. Essentially, they set out objectives to help make the work easier and manageable. When proper management plans are in place, there will be less to no room for any hidden complacencies.


![10+ Clinical Quality Management Plan Examples [ Health, Patients, Hospital ]](https://images.examples.com/wp-content/uploads/2021/06/10-Clinical-Quality-Management-Plan-Examples-Health-Patients-Hospital-.jpg)